UnitedHealth Group reported first-quarter results Tuesday, revealing challenges facing the managed care industry. The managed care giant posted revenue exceeding $100 billion quarterly, reflecting scale and diversification. Earnings per share beat analyst expectations marginally, but guidance disappointed investors seeking more optimism.
Junior broker from Nummvix breaks down how medical cost trends remained elevated concern pressuring profit margins. Utilization patterns are normalizing from pandemic disruptions, creating expense headwinds across the membership base. Profit margins compressed from historical peaks as healthcare inflation persisted despite broader economic moderation.
The Revenue Growth
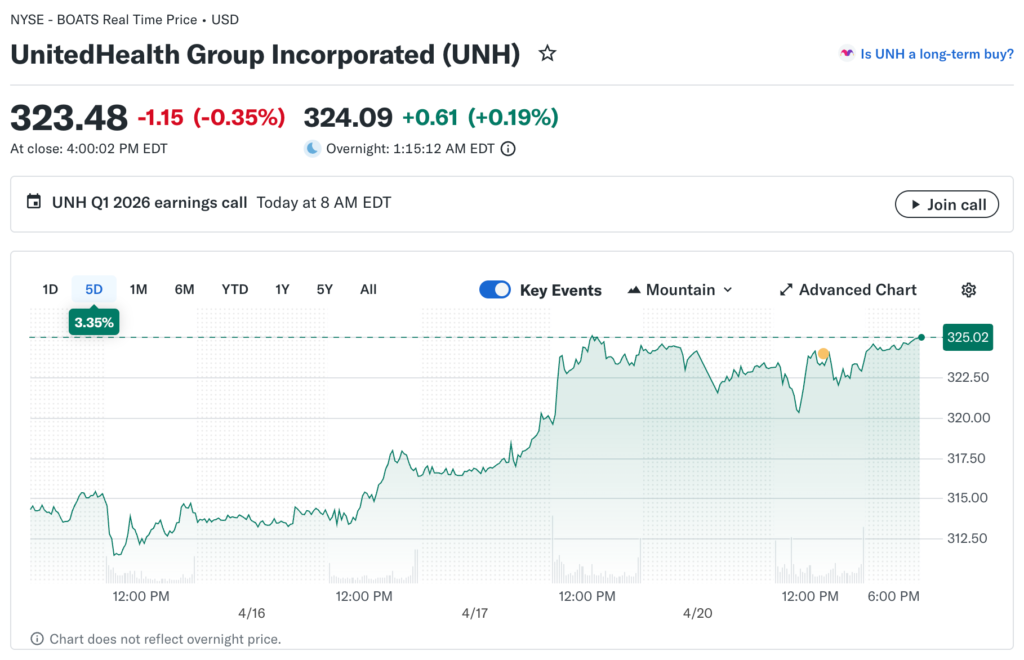
Total revenue increased 8% year-over-year, driven by membership expansion and premium rate actions. The membership growth across all segments, including commercial, Medicare, and Medicaid populations. Premium increases contribute substantially to offsetting rising medical costs only partially.
The UnitedHealthcare insurance division is leading gains with strong enrollment trends in major markets. The Medicare Advantage enrollment is up 6% annually as baby boomers age into the program. Commercial membership is stable despite a tight labor market, supporting employer-sponsored coverage continuation.
Optum health services growing faster than the insurance segment, demonstrating strategic diversification success. The physician practices expansion, continuing with the value-based care model, and gaining traction. Data analytics businesses are performing well as healthcare providers seek efficiency improvements.
The Medical Costs
Medical loss ratio at 83.5% for the quarter is higher than the targeted range of 82-83%. The claims costs are higher than anticipated, with utilization accelerating unexpectedly. Utilization trends are reverting to normal after pandemic-era suppression, creating a catch-up effect.
Deferred care from the pandemic is catching up as patients address postponed procedures and treatments. The elective procedures volumes are increasing, straining the cost structure. Chronic disease management is intensifying as complications from delayed care have emerged, requiring expensive interventions.
Pharmacy costs are rising from the GLP-1 drugs revolutionizing obesity and diabetes treatment. The obesity medications are driving spending with widespread adoption among eligible populations. Specialty pharmacy is growing rapidly, accounting for an increasing share of total drug spending.
The Medicare Business
Medicare Advantage margins under pressure from multiple directions, squeezing profitability. The Star ratings are impacting bonus payments, with quality measures becoming more stringent. Quality metrics require investments in care coordination and preventive services.
Government reimbursement rates are insufficient, argued management, citing medical cost inflation. The medical inflation exceeding rate updates are creating structural profitability challenges. Profitability is declining in the segment despite revenue growth as the economy deteriorates.
Competitive intensity is increasing for enrollment with aggressive marketing and rich benefits. The benefits of richness are driving share gains but compressing margins significantly. Marketing costs elevated during the annual enrollment period, stretching budgets.
The Commercial Segment
Employer-sponsored coverage is supported by steady membership and strong labor market fundamentals. The labor market strength supporting enrollment as employment remained near historic highs. Group business fundamentals solid with renewal rates favorable.
Self-funded clients are growing in share as large employers assume more risk directly. The administrative services only model generates fees without underwriting risk. Risk transfer to employers, changing revenue mix, but reducing volatility.
Pricing discipline was maintained rigorously, with underwriting selection careful to preserve margins. The renewal rates up mid-single digits, reflecting medical cost inflation pass-through. Underwriting selection careful avoiding adverse risk as competition intensified.
The Medicaid Operations
Medicaid membership is fluctuating with the eligibility redetermination process ongoing across states. The redetermination process is ongoing after the pandemic-era continuous enrollment ended. Enrollment is declining from peaks as eligibility is verified, creating revenue headwinds.
State budgets are constraining rate increases despite rising medical costs squeezing margins. The reimbursement inadequate for costs in many markets, creating losses. Profitability challenges in the segment are prompting a strategic review of participation.
Contract wins in new states offsetting losses elsewhere with a geographic diversification strategy. The geographic expansion strategy balanced portfolio risk across different regulatory environments. Diversification across regions mitigates concentration risk from adverse state actions.
The Optum Performance
OptumHealth’s value-based care is growing rapidly, with physician group acquisitions continuing. The physician groups are expanding their footprint in attractive markets with aging demographics. Risk-based contracts are increasing their share of revenue, aligning incentives for cost management.
OptumInsight technology and services are strongly benefiting from digitization trends in healthcare. The data analytics demand is robust as providers seek to improve operational efficiency. Revenue cycle management solutions are gaining adoption, addressing the administrative burden.
OptumRx pharmacy benefits management is performing well despite competitive pressures intensifying. The mail-order volumes are growing with convenience and cost advantages driving adoption. Specialty pharmacy high margin business growing faster than traditional pharmacy.
The Sector Implications
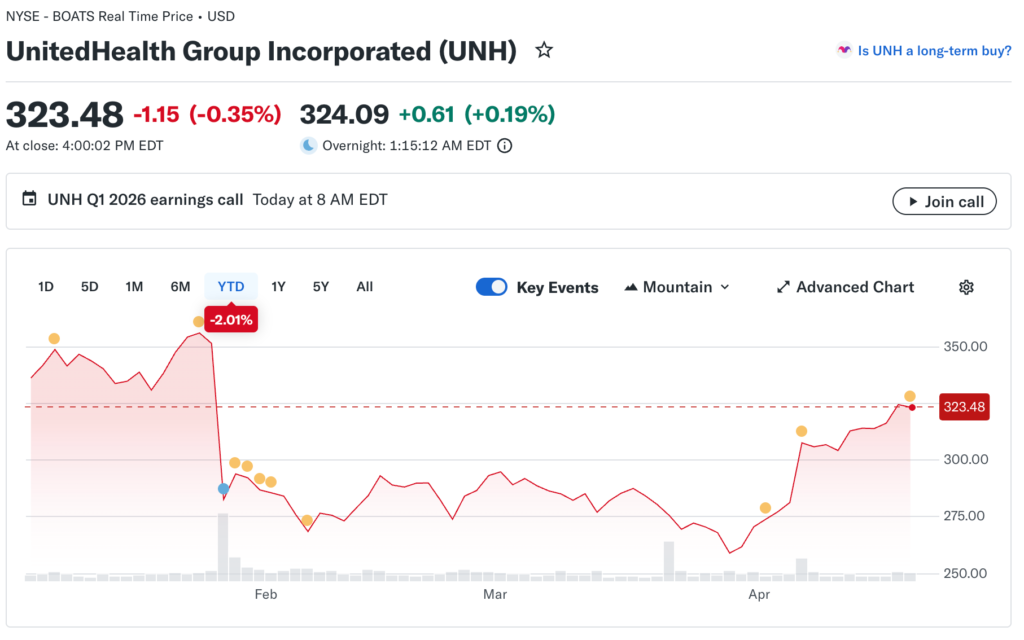
Managed care stocks trade together with high correlation within the group. The correlation within the group is high as systemic issues affected all. Systemic issues affecting all players are limiting differentiation opportunities.
Hospital operators are benefiting from utilization recovery, with procedure volumes strong. The procedure volumes are driving revenue growth for hospital systems. Payer mix improving as commercial and Medicare share increased.
Pharmacy stocks received mixed reactions to trends, with drug pricing debates ongoing. The drug pricing debates are ongoing, creating regulatory uncertainty. Biosimilar competition is increasing for specialty drugs, pressuring pricing.
